Training against medical errors
Surgical simulations can save lives, Anja Behringer reports Medical errors occur more frequently than traffic accidents and clearly better systems are needed to improve patient safety. Thus the importance of medical training using human simulation models is increasingly emphasised in Germany.
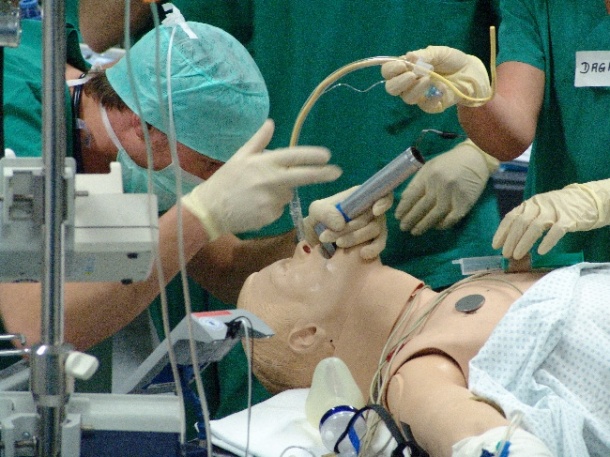

Having extensively studied the causes (and particularly human factors) of medical errors, Dr Marcus Rall heads the Tübingen Patient Safety and Simulation Centre (TÜPASS) at the University Hospital in Tübingen ‘Simulator training is not an obligatory part of training, which is why only individuals attend. However, it is more effective to train the whole team to establish a safety culture. This also promotes motivation and a good working atmosphere in the hospital.’ Just how important he considers this preparation is demonstrated by his work and involvement, amongst others, with the Society of Simulation in Healthcare and the European Society of Anaesthesiology (ESA), for which he heads the subcommittee on Patient Safety.
Faced with today’s simulator trainee doctors see not only a real looking human form, but one that can blink, has pupils that react to light and also reacts to around 80 types of medication as a real human would. Vital functions are realistically displayed on monitors in the same way this is done in an operating theatre or an intensive care ward. The surgical teams practise dealing with emergency situations with a particular focus on the decisionmaking process, as effective communication within the team is vital – bearing in mind that hierarchical structures can also be the cause of incidents.
The surgical scenarios are not only instructive for trainees but expert medics can also use them to practise rare surgical techniques or crisis situations. Team training is compulsory in aviation tuition and other elements from the world of aviation, e.g. checklists and safe communication, are taught as part of the simulator training at the Interdisciplinary Medical Simulation Centre in Dresden University of Technology (ISIMED), from which a team visits hospitals to train in patient safety. Acknowledging critical incidents and near misses, clarifying the causes of those events and thus avoiding mistakes and potential harm for patients has become a
central topic for in- and out-patient care.
One way to achieve this is the use of error reporting and training systems for critical events: Critical Incident Reporting Systems (CIRS). So far, these reporting systems have only been used either within institutions or on a national level. Therefore, in partnership with healthcare institutions in Berlin, the Berlin Chamber of Physicians and the Agency for Quality in Medicine have founded the regional network CIRS-Berlin. This offers participants in the project the opportunity to collate information on critical incidents and near misses in a joint reporting pool. To ensure potential errors do not even occur, the World Health Organisation WHO) has compiled a simple safety checklist, which may initially appear banal, but is actually based on the most common treatment errors that occur – with serious, negative results for the patients.
To assess the effect of the list, members of the Safe Surgery Saves Lives Study Group examined the treatment history of 7,688 non-cardiac surgery patients aged over 16 years, in eight socially and technologically different hospitals, for three months prior to (3,733 patients) and three months after (3,955 patients) implementation of the list.
The main results, published in the New England Journal of Medicine (MEJM) conclude: The rate of all significant complications during treatment and 30 days after treatment decreased statistically significantly from 11% before the use of the list to 7% afterwards; mortality during and after surgery fell from 1.5% to 0.8%. Cases of postoperative infections and the need for unplanned, further surgery also decreased significantly. This success was seen in all social settings. Hospitals took between a week and a month to integrate the checklists into their daily workflows. Experiences in hospitals with different organisational structures have shown that the introduction of these safety checks costs neither a lot of money nor time.
20.12.2011